Diabetes Data Cell: From fragmented data to a national policy tool
Fragmentation of diabetes data poses several challenges across member states. Tackling this issue is a key step towards transforming fragmented diabetes data sets into actionable evidence for smarter health policy. Within JACARDI’s Work Package on Data, the Diabetes Data Cell Project is being developed by Sciensano. The Belgian institute for public health aims to address this question in an effort to optimise patient and healthcare data alignment. The project has recently reached a major milestone: approval by the Belgian Data Protection Authority to link individual-level primary care and specialist clinical datasets with national administrative data on reimbursed healthcare use.
A first data flow covering 2017-2024 has already been completed, resulting in a linked dataset of 76,965 unique individuals living with diabetes across care settings in Belgium. The full governance framework, including legal approvals and secure linkage procedures, has been established and was submitted in December 2025 for publication to BMC Public Health journal. “This marks a crucial step toward building Belgium’s first comprehensive national diabetes dataset,” explain the authors, Astrid Lavens, senior researcher and pilot project coordinator, Kalina Todorova, junior researcher, and Margot Buyle, senior researcher.
What makes this initiative truly unique is how people living with diabetes are identified. Rather than relying on proxy indicators such as therapy use or reimbursement codes, individuals are selected based on the clinical diagnosis recorded in the electronic patient records by their healthcare provider. This ensures a far more accurate and clinically meaningful population definition, a strong foundation for robust real-world evidence.
Primary analyses have already generated valuable insights, such as mapping the overlap between primary and specialist clinical databases and identifying how patients move across levels of care. “For the first time, we can follow individuals across the healthcare system and connect clinical information with data on healthcare utilization and reimbursement,” explain the members of this pilot.
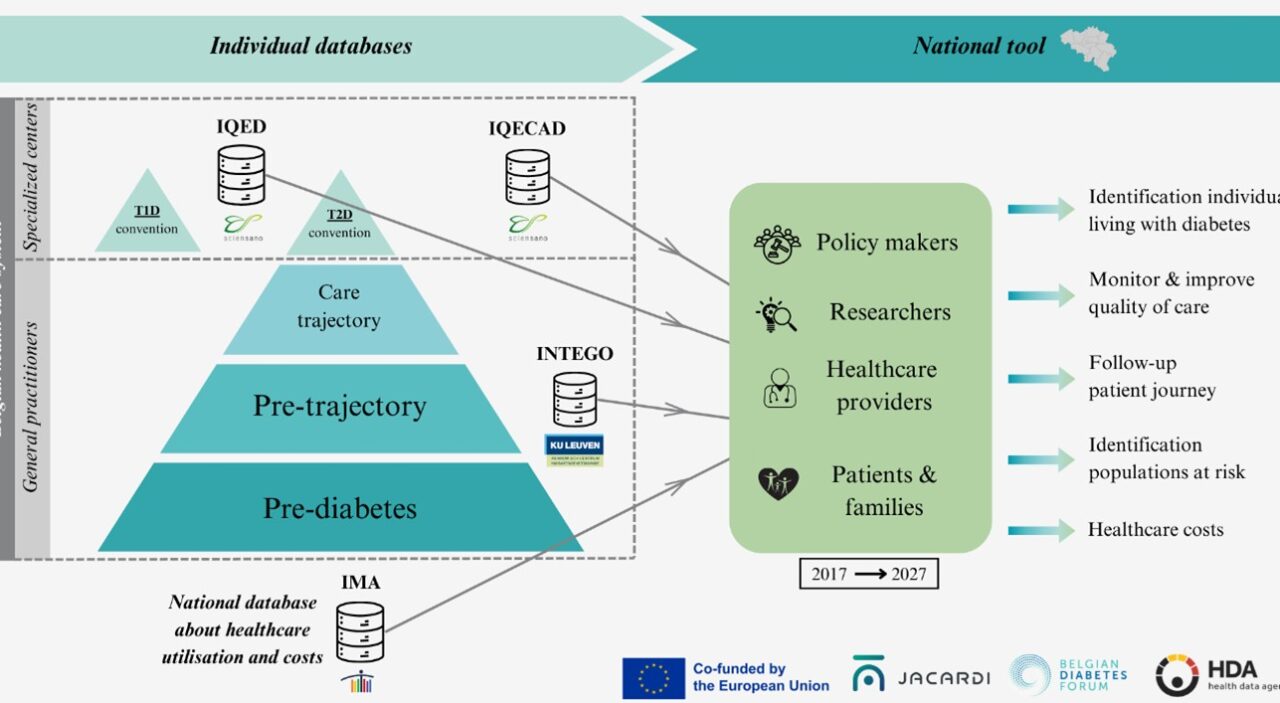
The next phase brings together three institutions: Sciensano, KU Leuven and the Intermutualistic Agency (IMA); each contributing complementary expertise in clinical epidemiology, health services research, and administrative data analysis. By combining these strengths, the consortium – together with the Belgian Diabetes Forum (BEDF) – will transform this linked dataset into a powerful tool for evaluating care quality, treatment patterns, patient pathways, outcomes, and costs.
The Diabetes Data Cell is more than a technical exercise in data linkage. It is a concrete step toward evidence-informed diabetes policy, supporting better planning, improved quality of care, and more efficient resource allocation. By turning routinely collected data into integrated, policy-relevant evidence, this project demonstrates how collaboration within JACARDI can directly strengthen chronic disease monitoring and decision-making at national level, with potential lessons for other countries and other non-communicable diseases.